Effects of Covid-19 on the cardiovascular system
A research team led by Yvonne Döring has published an overview of the current state of knowledge about short- and long-term effects of SARS-CoV-2 on the cardiovascular system.
Early on in the pandemic, it became clear that SARS-CoV-2 was not limited to respiratory infection but could also be found in other tissues, including the vascular system. It was also soon known that people with pre-existing conditions such as diabetes and hypertension were more likely to suffer severe Covid-19 symptoms and more likely to die. In addition, severely ill Covid-19 patients have clinical symptoms such as hypercoagulation, cardiomyopathy, cardiac arrhythmias and endothelial dysfunction, suggesting involvement of the vascular system in Covid-19 pathology.
The research team from Bern University and Inselspital Bern, led by Yvonne Döring, Britta Engelhardt, Nadia Mercader and Robert Rieben, have now brought together all available scientific knowledge about the effects of SARS-CoV-2 on the cardiovascular system in a review article in the journal Frontiers in Cell and Development Biology.
Pre-existing cardiovascular conditions such as hypertension and high cholesterol levels are risk factors for severe disease. In addition, about one-third of all Covid-19-related deaths have a history of cardiovascular disease. The reason for this could be the receptor ACE2, which is the main entry port for SARS-CoV-2. ACE2 is not only found in the lungs, but has also been detected in tissues of the intestine, the nose and the cardiovascular system. Although heart muscle cells tend to have fewer ACE2 receptors, ACE2 expression almost doubles in advanced cardiomyopathy. It has also been observed that the ACE2 receptor is more highly expressed in people with diabetes.
Cell culture experiments and experiments in animal models also showed that heart muscle cells can indeed be directly infected. The extent to which this also applies to human mature cardiac muscle cells still needs to be investigated in more detail. Whether endothelial cells of blood vessels can also be directly infected or are mainly damaged by the SARS-CoV-2-induced immune response and the subsequent inflammatory reaction has also not yet been adequately investigated.
Besides acute symptoms and the question which cell type other than lung epithelial cells can be directly infected by SARS-CoV-2, public interest in the consequences of long COVID disease is also growing. In long COVID, cardiovascular system impairments are often observed in addition to fatigue. For example, two to six months after being ill with Covid-19, 5-21% of all patients reported chest pain. Heartbeat irregularities and palpitations have also been increasingly written about. However, there are still too few studies on this and, in particular, insufficient data over a longer period of time and with a large number of participants.
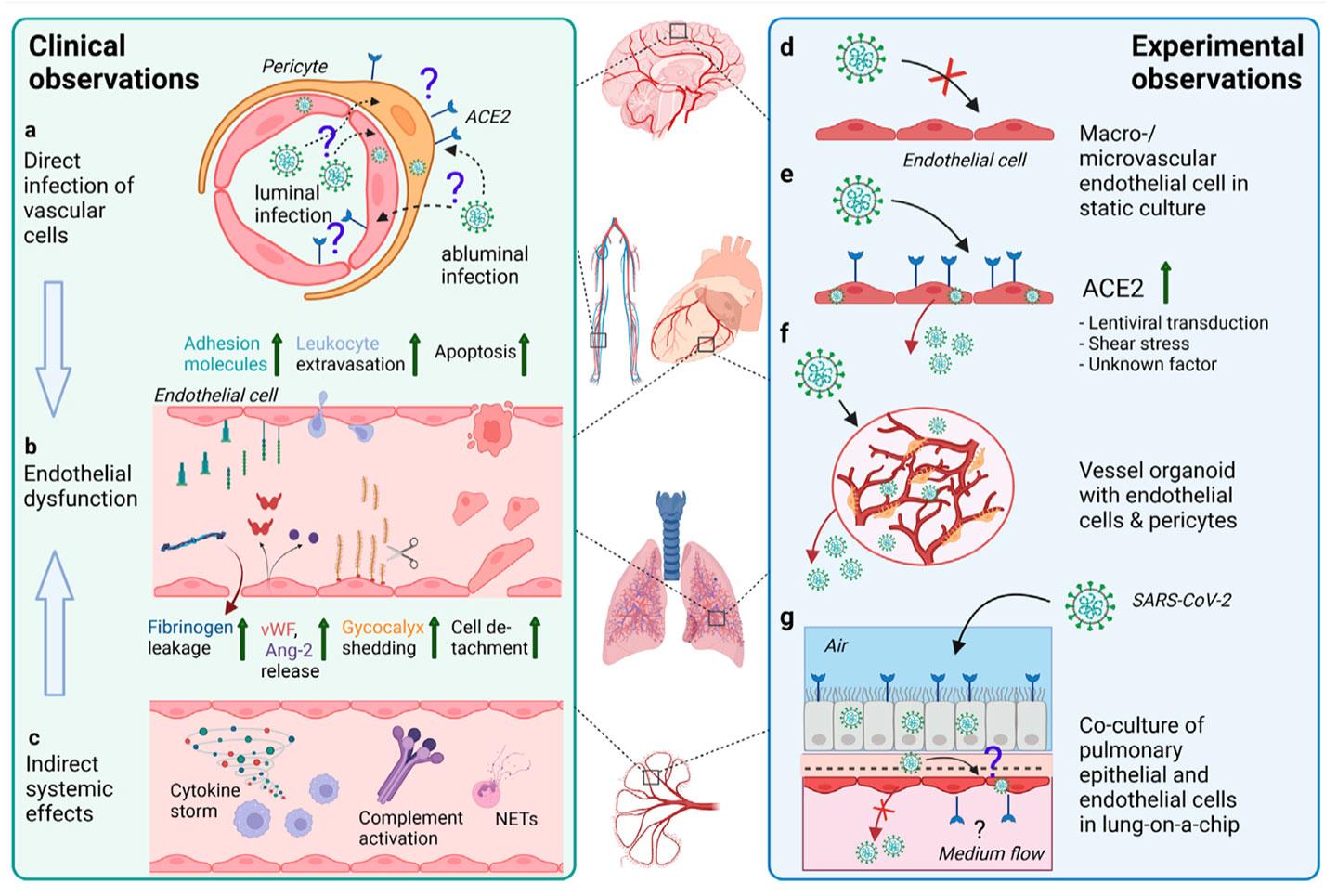

The article provides a detailed overview of the current knowledge about Covid-19 and its impact on the cardiovascular system. It highlights the need for concerted efforts to understand the direct and indirect cardiovascular effects of SARS-CoV-2 infection as well as its longer-term consequences, thereby paving the way for new treatment strategies.
Project description: Consequences of SARS-Cov-2 infection in cardiovascular disease
